Disclaimer: This article on Hysterectomy is meant to be a source of valuable information for the reader. However, it is not a substitute for direct expert assistance. Please seek help from a medical professional to learn more in-depth details of this procedure.
The uterus is responsible for a lot of functions in the female body. From menstruation to fertility, and even pregnancy, this pear-shaped organ is critical in keeping a female healthy. However, what if this organ becomes engulfed in severe pain over time? Or in the worse case, develop into cancer?
One major option for people assigned females at birth (AFAB) can consider is getting a hysterectomy.
Take a deeper dive into this surgical operation, why people go through it, and tips on preparing and recovering healthily.
What is a Hysterectomy?
Healthline defined Hysterectomy as:
“A surgical procedure that removes the uterus, where pregnancy takes place. Your uterine line will also be affected, where menstruation occurs.”
Cleaveland Clinic added that in some cases, the cervix might be removed depending on the degree of your reason for getting a hysterectomy. Regardless, pushing through with this operation has a bunch of benefits. One, it can save someone’s life and/or improve their lifestyle. Another is that it can reduce chronic pelvic pain and abnormal bleeding.
But before proceeding with this operation, you need a doctor’s referral to do this procedure. Because once you proceed with this procedure, you cannot get pregnant and have menstrual cycles. You’ll also go into menopause immediately if you also choose to have your ovaries removed.
Why Do People Have a Hysterectomy
There are various reasons why people choose to have a hysterectomy. Although this procedure for non-cancerous reasons is only considered when other alternatives prior didn’t work out. Regardless, we gathered all the possible reasons why people would choose to get a hysterectomy.
1 Cancer

Cancer is a common reason behind getting a hysterectomy, specifically in areas such as the uterus, cervix, ovaries, and fallopian tubes. Healthline advised that how you’ll move forward with this procedure depends on the type of cancer you have and how advanced it is. Before considering this option, radiation and chemotherapy are attempted first.
Although there have been instances where removing your uterus is done to prevent one from getting cancer, or there are suspicions that you might have one. It’s better to beat it before getting it.
2 Uterine fibroids

Also called myomas, these fibroids are non-cancerous tumors that are formed in the uterus. These result in being another common reason why people get a hysterectomy because they cause heavy menstrual bleeding and pelvic pain, even affecting one’s fertility.
Your doctor may recommend birth control pills as medication or doing a less invasive procedure like a myomectomy (removal of fibroids) first. But if they aren’t successful, that’s when you have the choice to get a hysterectomy.
3 Adenomyosis

This condition occurs when one’s uterine lining extends and grows into the muscle of the uterus. This makes one’s uterus thicker, resulting in heavier, painful menstrual flows. Usually, this condition could go away after menopause. But if not, hormonal treatments are an option at the start. If they don’t work out, a hysterectomy can be done.
4 Endometrial Hyperplasia

Getting this condition means your uterine lining thickens abnormally due to an increase in estrogen and not enough progesterone. It occurs during or after menopause and leads to heavy bleeding. It also increases your chances of being diagnosed with endometrial and uterine cancer.
5 Delivery Complications

In some situations, getting a hysterectomy within 24 hours after giving birth vaginally or through C-section is possible. This would be done as an emergency operation due to severe bleeding. Although it’s a rare occurrence, doing this would be life-changing for the mother.
6 Placenta Accreta

Also in line with pregnancy and delivery, this condition is when the placenta grows beyond the uterine wall. The severity of this condition would lead to a c-section operation, followed by a hysterectomy to lessen the blood loss from separating the placenta. This condition also shows no symptoms, so it’s best to pay close attention to your health and state.
7 Abnormal or Strong Vaginal Bleeding

If your menstrual flow tends to be strong and heavy, pushing through with a hysterectomy may be your best bet. Changes in hormone levels, infection, cancer, or fibroids can cause such bleeding, which can cause discomfort and pangs of pain. Hormone therapy may have been recommended initially, but it may not be enough to relieve the pain. Hence, going forth with a hysterectomy occurs.
8 Uterine Prolapse

This condition happens due to the stretching and weakening of pelvic floor muscles and ligaments until they falter to support the uterus. As a result, it slips down or creates a bulge in one’s vagina.
One would experience symptoms such as bladder issues, pelvic pressure, and bowel problems. Depending on the degree of the prolapse, a hysterectomy would be needed if the pelvic muscles have weakened drastically.
9 Endometriosis

This common health problem occurs when tissue sharing similarities to one’s uterine lining grows outside of the uterus or on other organs close to it. The most common places aside from the uterus it can grow are the ovaries, fallopian tubes, or any tissues surrounding the uterus. This health problem leads to extreme pain and irregular periods, even infertility
A hysterectomy is done only if hormonal therapy or any medical procedures to remove the endometrial tissues aren’t effective enough. And although a hysterectomy can reduce or alleviate the symptoms of this health problem, it’s possible to get it again. Thus, be in constant communication with your doctor about this situation.
10 Gender-Affirming Surgery

Someone who identifies as a transgender male or non-binary can get a hysterectomy to further align with their identity. It’ll also make them feel more authentic and embrace themselves more. We’ll further discuss what types of hysterectomy to decide from, but one can decide to remove their uterus only or also include their fallopian tubes and ovaries.
Types of Hysterectomy
When you discuss with a medical professional, you can either remove all or part of your uterus. It’s important to take their recommendations and learn the benefits and risks of each procedure. Learn more about those choices of Hysterectomy below.
1 Total Hysterectomy
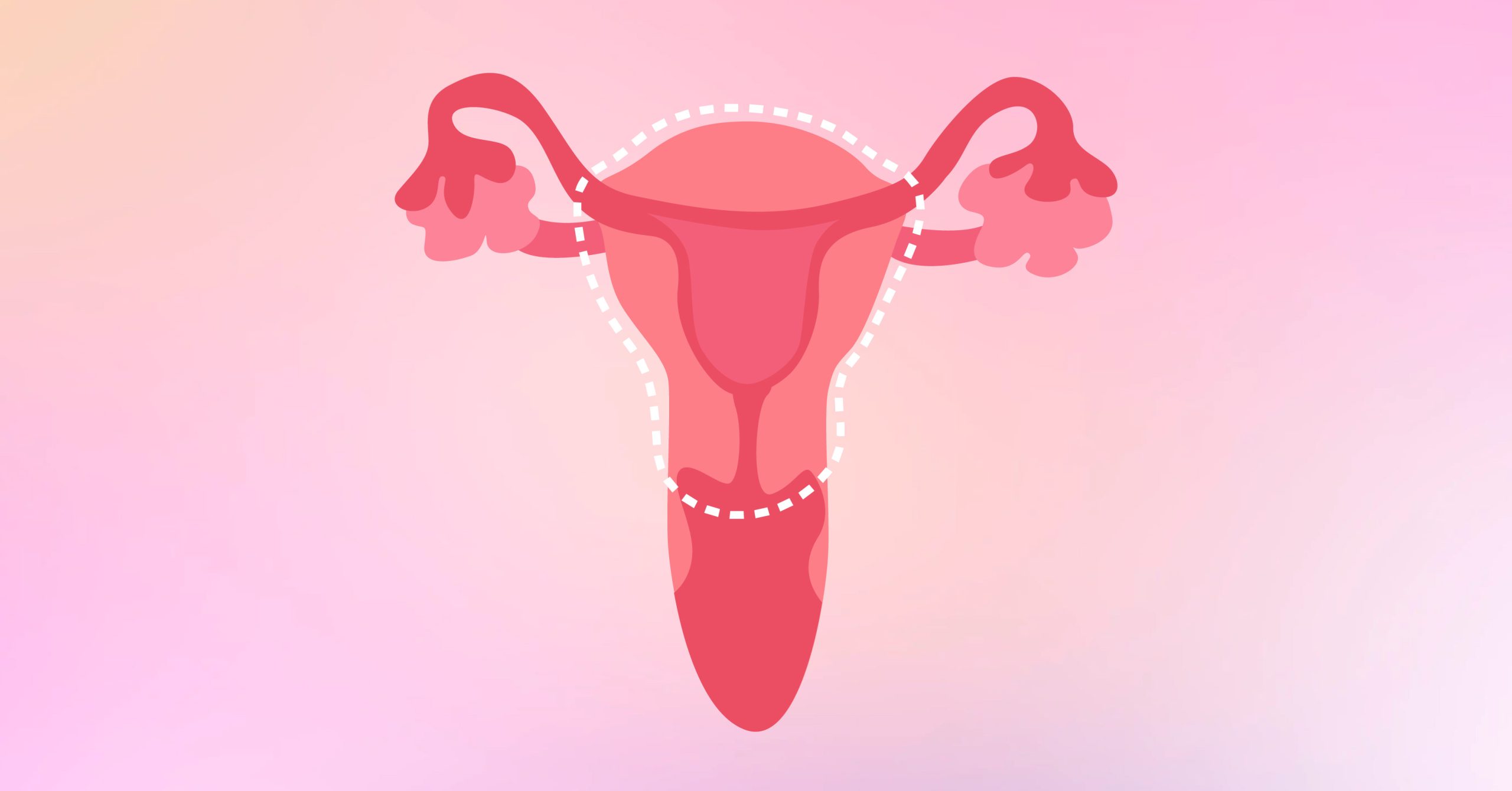
This type of hysterectomy means that you’re choosing to remove all of your uterus. This also includes your cervix. Your ovaries and fallopian tubes may or may not be removed as well, depending on what you discuss with your doctor. According to Healthline, they added that you must continue having regular pelvic examinations post-hysterectomy.
2 Partial Hysterectomy
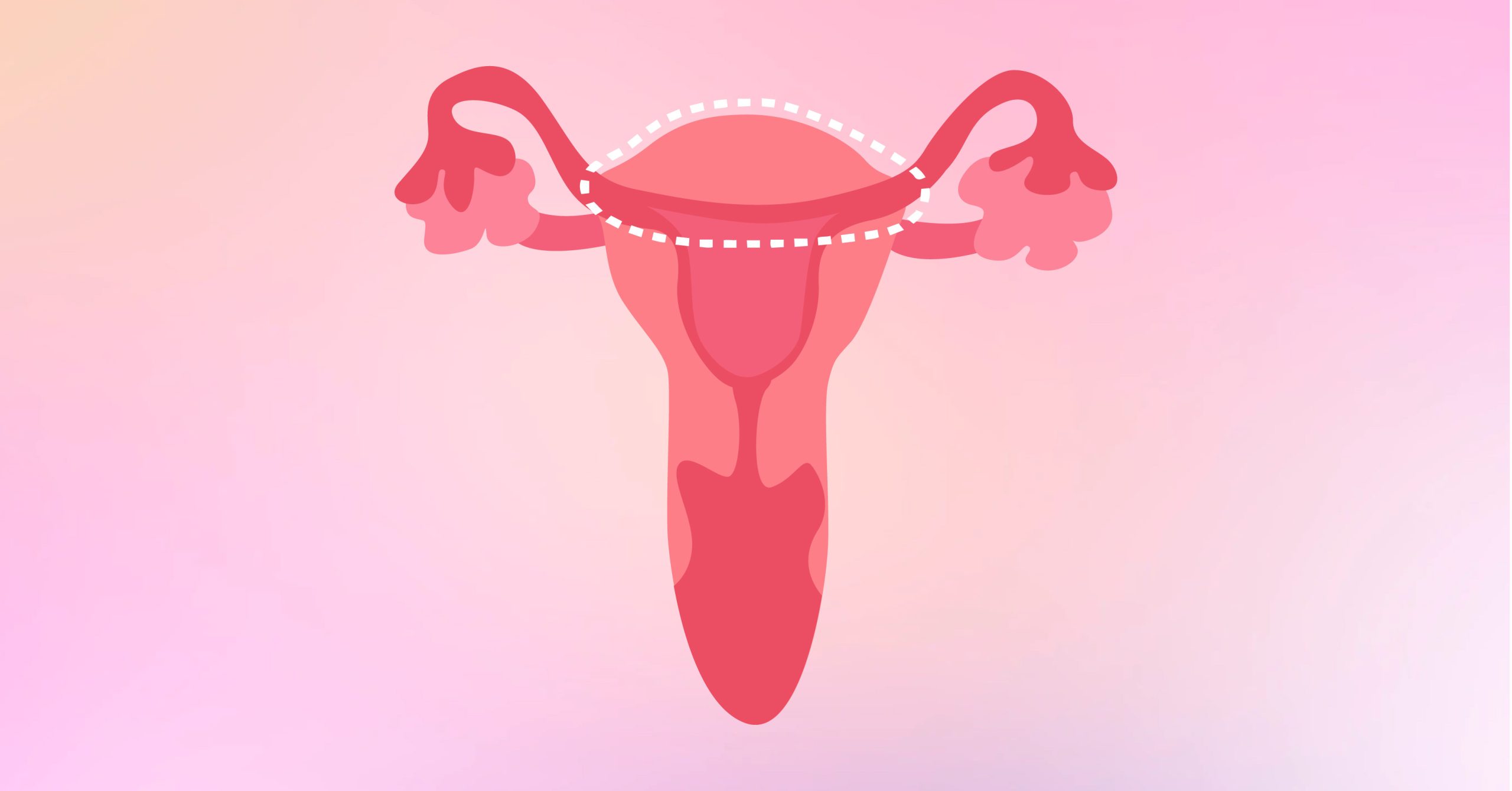
Also known as Supracervical or Subtotal Hysterectomy, this type of hysterectomy only removes the upper part of the uterus. Your cervix is left intact, still with the choice to remove your ovaries and fallopian tubes or not.
3 Total Hysterectomy with Bilateral Salpingo-Oophorectomy
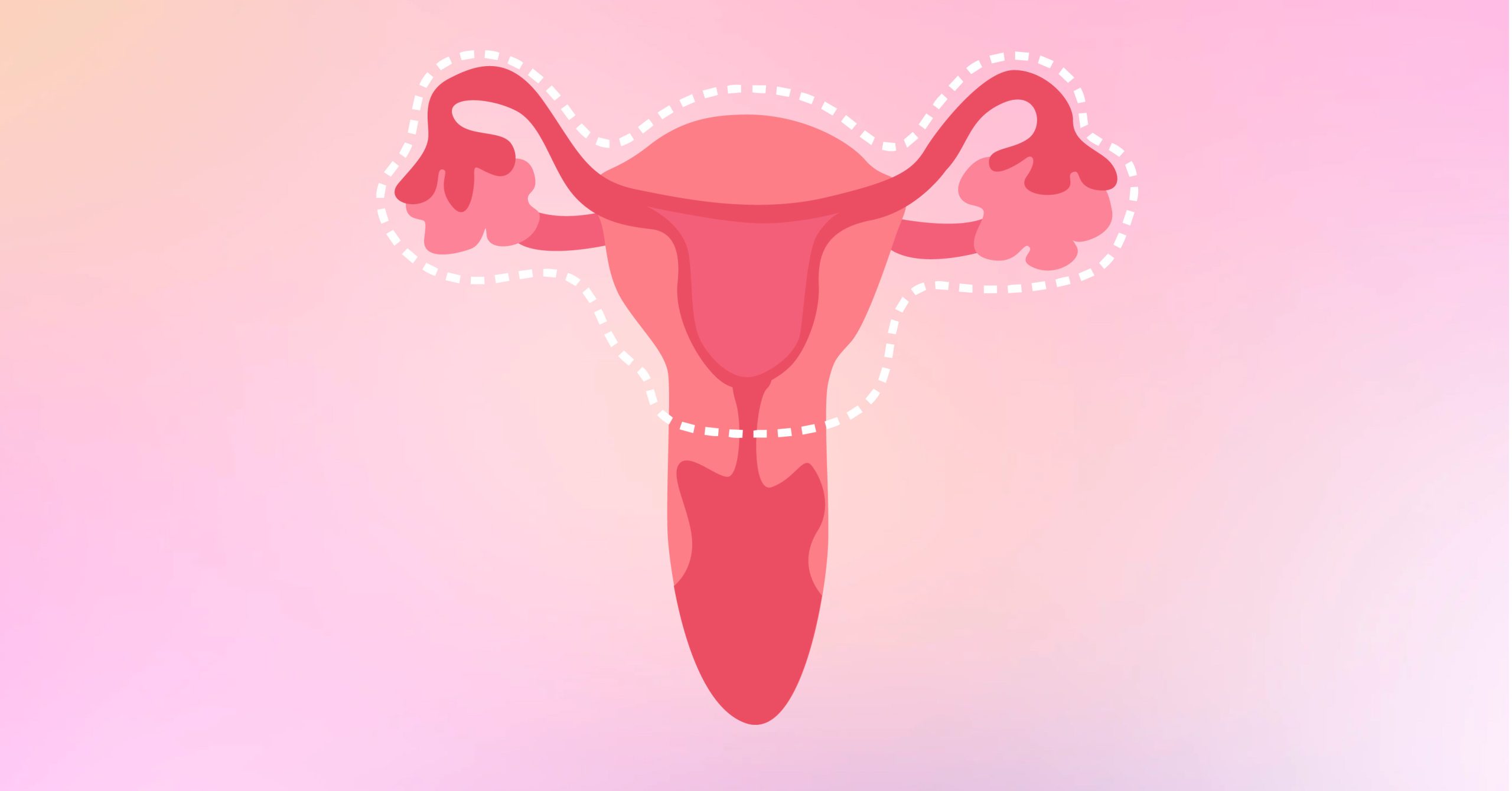
In this option, you’re going through 3 procedures in one go. As you have your uterus removed, you’ll also be removing your fallopian tubes (salpingectomy) and ovaries (oophorectomy). If you’re not yet experiencing menopause, that will change once your ovaries are removed.
4 Radical Hysterectomy with Bilateral Salpingo-Oophorectomy
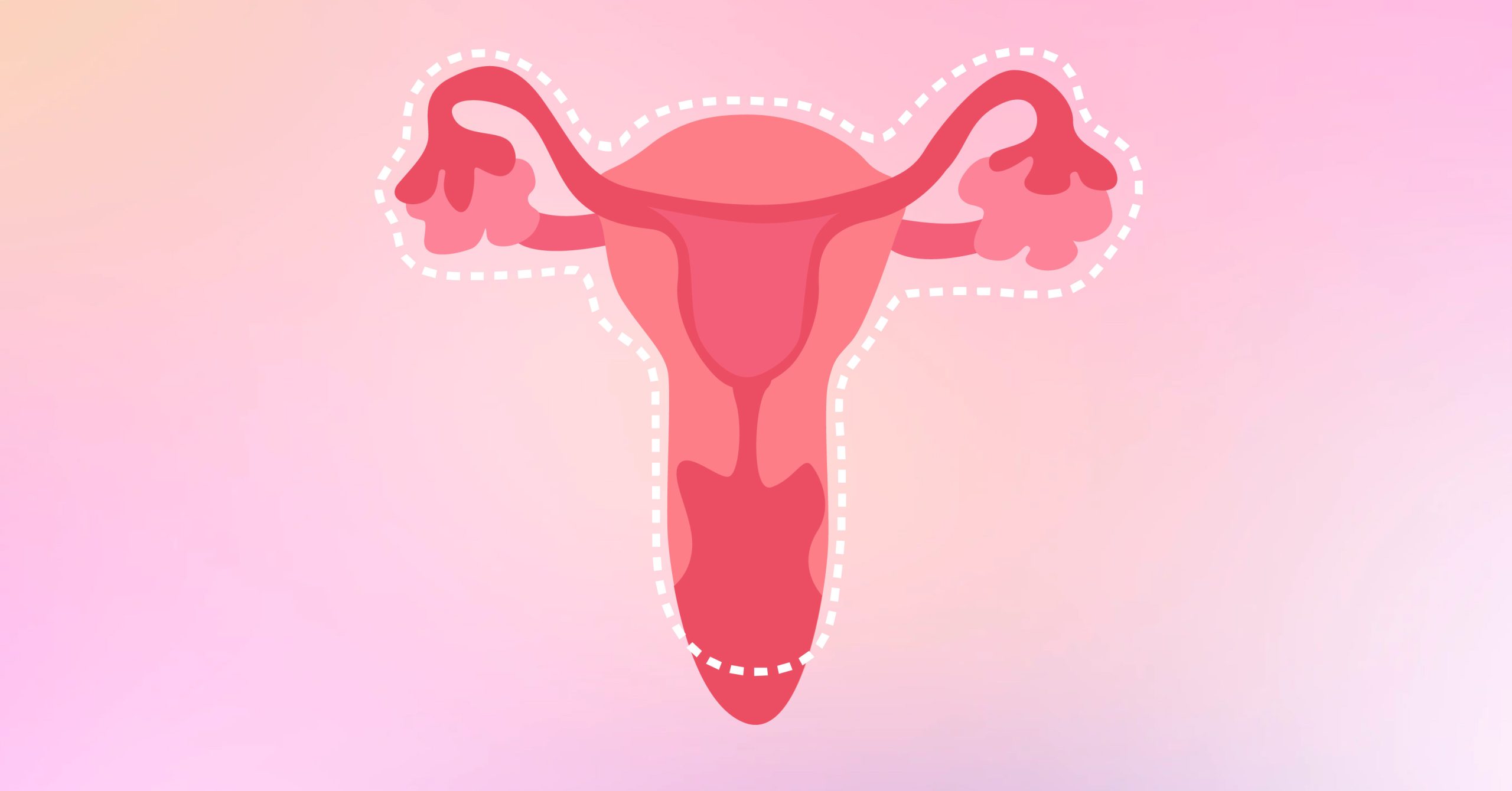
If you have cancer, this option may be suitable for you. In this type of hysterectomy, your uterus, cervix, and the upper part of your vagina, some surrounding tissue, and lymph nodes will be removed. This also applies to your fallopian tubes and ovaries with the other procedures mentioned.
Ways to Perform a Hysterectomy
A hysterectomy can either be a minimally-invasive procedure (MIP) or an open surgery for the patient. Let’s uncover more about these types and what approaches you can take with them.
1 Vaginal Hysterectomy

This minimally invasive procedure removes your uterus through an internal incision at the top of your vagina. This incision will leave no scar since it dissolves over time.
This procedure is done by those with non-cancerous conditions, such as uterine fibroids, uterine prolapse, and severe endometriosis. You can go home right after the procedure or stay in the hospital for 1-2 days for close monitoring. The recovery period can range from 3-4 weeks.
2 Laparoscopic Hysterectomy
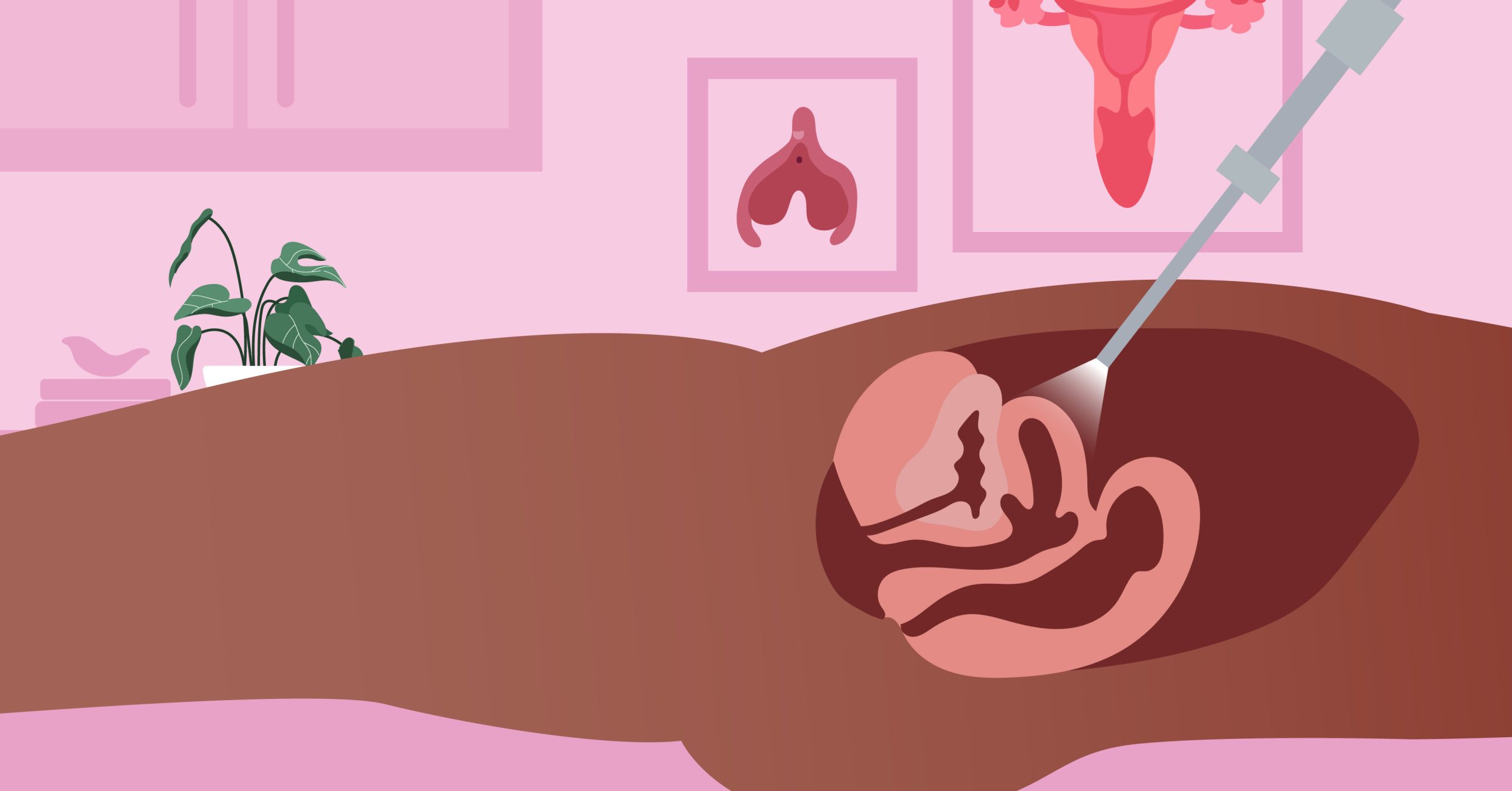
This is another minimally invasive procedure that requires a laparoscope inside your lower abdomen, a slender device with a video camera on the end. Due to this device, your pelvic organs can be seen through a screen by your doctor. This is followed by numerous small incisions made by other surgical tools to remove your uterus instead of one big incision. It can be done either in the abdomen or in the vagina.
Like the latter option, you can go home or stay for a few days in the hospital post-hysterectomy. Recovery is around 2-6 weeks.
3 Robotic-assisted Laparoscopic Hysterectomy

Similar to the previous procedure, the doctor in charge has the aid of a robot to carry out this procedure. WebMD adds that the surgeon utilizes a robotic system of surgical tools from outside the patient’s body. This system further allows the surgeon to use natural wrist movements to operate and take a clearer look at the hysterectomy on the screen.
4 Abdominal Hysterectomy

This procedure is a type of open surgery wherein your uterus is removed through a six-to-eight incision in your abdomen. This incision can be horizontal above your pubic bone or vertical by your belly button. Staples or stitches are used to close the incision. You may need to stay in the hospital a little longer (2-3 days), and recovery is around 6-12 weeks, depending on the size of the incision from the hysterectomy.
This procedure is also done with cancer is involved in the patient, when the uterus expands and/or the illness spreads in various parts.
Side Effects and Complications of Getting a Hysterectomy

Hysterectomy is a safe procedure, wherein 90% of patients having gone through that procedure live a longer life. This is in the case of patients with cervical cancer. However, side effects and some complications can arise along the way. Here are some of them to look out for before deciding on going under the cut.
- Blood clots
- Emotional distress
- Torn internal stitches
- Vaginal Prolapse
- Anesthesia-related issues
- Bleeding (hemorrhage)
- Weakness of muscles or ligaments that support the vagina, bladder, and rectum
- Chronic Pain
- Vaginal fistula formation
- Intestinal blockage due to scar tissue
- Loss of libido or sexual drive
- Lymphedema (buildup of fluid in the legs or abdomen)
- Damage in your ureter, bladder, and bowel
- Infection (e.g. urinary tract injury)
- Early Menopause (hot flashes, vaginal dryness, insomnia, etc.)
How to Prepare for a Hysterectomy
A hysterectomy can sound intimidating and scary, especially when there are risks side by side with benefits. But no worries, we have some key advice to lessen your fear and get you in the right mindset for your operation.
1 Fill up your knowledge.

Doing your research and preparing questions for your doctor regarding this procedure can definitely lower your nerve around it. Get quick information through deep research on the internet, and consult with your doctor with those questions about this procedure. Over time, ask your doctor which type of procedure and surgical method to follow the procedure that fits your situation as well. You may do the same with your surgeon so to be aligned with everything you need to know.
2 Be transparent with your medication history.

When meeting with your doctor, it’s encouraged to inform them of any medication you’re taking at the moment. That way, they can determine whether or not you should continue taking them or pause for a while before the procedure. This is because it could meddle with the anesthesia, especially if you’re going to have an open abdominal hysterectomy.
3 Quit your vices, even just momentarily.

As much as possible, you have to be healthy before your scheduled hysterectomy. So if you’re a smoker, pack away your nicotine. Social drinker? You may need to turn down that invite to hang out with your friends unless you can join them without drinking at all.
Oh, you do both? Cut them off, even for a bit until you’re done and recovered from your operation. Take this chance to also follow a healthy diet and active lifestyle to further prepare your body.
4 Discuss anesthesias with your doctor.

After deciding on what kind of hysterectomy to use, your doctor will talk through the kind of anesthesia you’ll have during the procedure. It can either be general (you’ll be asleep the entire procedure) or regional (the medication is inserted near the nerves of your lower back to “block” any pain as you stay awake). The latter is also known as an epidural or spinal anesthesia, the same one used during childbirth. Knowing this is important so you can further prepare yourself for the day of the operation.
5 Plan out your hospital stay beforehand.

If you choose to stay in the hospital for a night or two, even if your operation is a MIP, cooperate with your doctor when to do this surgery. If you’re also concerned about work, plan your operation during the weekend, so you have enough time to rest.
For those choosing an abdominal hysterectomy, you’ll require more time to stay in the hospital, so communicate with both your doctor and your workplace. For the latter, request a long leave period so you can recover better. Especially since it’s health-related, you can make compromises and such. As for the former, pass on whatever you discuss with your workplace, then find a suitable period to do the operation.
6 Ask for assistance after the procedure.

You’ll be on medications post-hysterectomy to ease your recovery period, alongside other restrictions. Before that, task someone (a partner, friend, or family member) to take care of you. It’ll take a while to drive again, so have them drive you home if you go somewhere (not work-related!). Also, ask for their help fix your place and other household chores on days your body urges you to rest more in bed. If you live with someone, that’s even better.
Tips on Recovery Post-Hysterectomy
After going through a hysterectomy, you’ll be required to have a period of recovery before returning to your normal lifestyle. Here are some important tips we gathered to ensure a smooth sailing recovery post-hysterectomy.
1 Get plenty of rest.

A hysterectomy is a surgical procedure wherein your entire body will be affected even if only a certain part was fixed. So make sure to hit the hay earlier or even nap within the day so your body can repair and re-energize from that tedious operation. It will also improve your mood and reduce your stress levels.
2 Don’t carry anything heavy.

It’s a no-brainer that you’ll be sore and tired during your recovery period from a hysterectomy. So simultaneously, avoid lifting items that are more than 10 pounds. Bending is also bad for you during this time, so as much as possible, ask for help if you live with other people or have someone take care of any hard task.
3 Stock up on sanitary pads or panty liners.

You’ll experience light bleeding for a while post-hysterectomy, so wearing any of these products will collect the discharge. It’ll also prevent your clothes from getting any stains. Avoid tampons since you’ll have to stick that up your vagina, which is highly discouraged.
4 Wait at least 6 weeks to engage in sexual intercourse or activities.

As much as possible, putting anything inside your vagina is prohibited until your doctor says so. That includes any external organ (fingers, tongue, etc.) or item (sex toy) up there. Because think about it — if you went for a vaginal hysterectomy, your body is still recuperating from the devices inserted and what they did to your body. Patience is a virtue, but you got this.
5 Stick to a light exercise routine.

Even while recovering, incorporating active movement into your lifestyle would benefit your body. Take short walks during this time, then build up your daily distance to challenge your body. Light movements can still make a big change in the long run.
Frequently Asked Questions

Still curious to know more about a hysterectomy? Well, you’re in luck! We answered a few common inquiries to further widen your knowledge on this life-changing procedure.
1 How long will the entire procedure of getting a hysterectomy take?
It can last between 1-4 hours.
2 Should I still have a Pap Test even after getting a hysterectomy?
It depends. If you have low risk of getting cervical cancer, it’s a no. But if you had a hysterectomy because of cancer, resume getting checked via Pap test.
3 Can I take a shower post-hysterectomy?
Yes. Gently clean your incision with soap and water. And don’t worry too much about the stitches since they’ll fade in a matter of weeks.
4 Will a hysterectomy affect my sex life?
No. You’ll still be capable of having sex, but mind you that symptoms of menopause will arise if your ovaries are removed. Especially with low sex drive and vaginal dryness as some of them, we suggest using water-based lube for your future sexcapades post-hysterectomy and even having an orgasm.
5 What organs will take place in that empty space?
After a hysterectomy, your small and large intestines will take up most of the space.
Takeaway
Even with its risks and side effects, getting a hysterectomy has been life-changing for many females. With the various options of this procedure, there’s a type that fits each situation out there. Just make sure to be in close contact with your doctor to further learn more about this procedure and what option suits your needs most.